Past pandemics
I’ve been reading about pandemics. The method was reading through this Wikipedia list: List of pandemics, and miscellaneous sources. The limitations of the method was that this list has a bias towards epidemics in the English-speaking world, that some of their figures were wrong, and that towards the end it tends to consider smallish pandemics. Moreover, there weren’t that many times where a disease was introduced to a new population and it had a low fatality rate (influenza being the chief example).
Some thoughts:
- Most pandemics throughout history had much higher mortality.
- Most pandemics had second, third waves, or lasted more than one year; the split was 42:18 (had second, third waves or lasted more than one year : didn’t). The two cases are often hard to differentiate.
- The split was 10/51 (and one ambiguous case) against a given pandemic becoming endemic.
- “Herd immunity” seems to be built over longer periods of time, rather than over the course of a year. Historically, one found out that there was herd immunity within a population because when the pandemic came back a decade hence, fewer and younger people died.
- Modern plagues can be thought as accelerated versions of older plagues; where it once took years from a pandemic to travel from China to Central Europe, it now takes day or weeks.
- Authorities and elites denying the extent of a plague, and this causing more pain and suffering… has been known to happen, and is even common.
- After a pandemic concludes, there might be some political will to do something so that this never happens again. This is relatively short-lived
CSV for the above here.
Some quotes from my notes:
“In overcrowded Athens, the disease killed an estimated 25% of the population. The plague returned twice more, in 429 BC and in the winter of 427/426 BC.”
“The physician to the Avignon Papacy, Raimundo Chalmel de Vinario (Latin: Magister Raimundus, lit. ‘Master Raymond’), observed the decreasing mortality rate of successive outbreaks of plague in 1347-8, 1362, 1371, and 1382 in his 1382 treatise On Epidemics (De epidemica). In the first outbreak, two thirds of the population contracted the illness and most patients died; in the next, half the population became ill but only some died; by the third, a tenth were affected and many survived; while by the fourth occurrence, only one in twenty people were sickened and most of them survived”
“a mortality rate of around 1%. Fernel and Paré suggest that the 1510 influenza “spread to almost all countries of the world” with the exception of the New World”
“These measures [were] enforced with harsh penalties including flogging and death” (about the 1592-1593 Malta plague epidemic)
A major outbreak in March 1630 was due to relaxed health measures during the carnival season (about the 1629–1631 Italian plague)
In Seville, quarantine measures were evaded, ignored, unproposed and/or unenforced. The results were devastating
Two suspicious deaths were recorded in St. Giles parish in 1664 and another in February 1665. These did not appear as plague deaths on the Bills of Mortality, so no control measures were taken by the authorities, but the total number of people dying in London during the first four months of 1665 showed a marked increase. By the end of April, only four plague deaths had been recorded, two in the parish of St. Giles, but total deaths per week had risen from around 290 to 398
Tobacco was thought to be a prophylactic and it was later said that no London tobacconist had died from the plague during the epidemic
Some people disputed the cause of the disease, and the doctor Giuseppe del Cosso insisted that it was not plague but a malignant pricking disease. Many went about their daily lives as usual, and this is believed to be a factor which resulted in such a high death toll. It was only after various European physicians gave their opinions that it was plague that strict containment measures were enforced, but by then it was too late
While at first the city authorities downplayed the plague, which had reached a peak in early October and then declined, this approach was abandoned when the death toll again started to rise significantly in November
In November 1709, when the Prussian king Frederick I returned to Berlin from a meeting with Russian tsar Peter the Great, the king had a strange encounter with his mentally deranged wife Sophia Louise, who in a white dress and with bloody hands pointed at him saying that the plague would devour the king of Babylon. As there was a legend of a White Lady foretelling the deaths of the Hohenzollern, Frederick took his wife’s outburst seriously and ordered that precautions be taken for his residence city. Among other measures, he ordered the construction of a pest house outside the city walls, the Berlin Charité.
In June 1710, most probably via a ship from Pernau, the plague arrived in Stockholm, where the health commission (Collegium Medicum) until 29 August denied that it was indeed the plague, despite buboes being visible on the bodies of victims from the ship and in the town
While Scania was protected from an infection from the north by a cordon sanitaire between it and Småland, the plague came by sea and made landfall not only in Västanå, but also in January 1711 in Domsten in Allerum parish, where the locals had ignored the ban on contact with their relatives and friends on the Danish side of the Sound, most notably in the infected area around Helsingør (Elsinore); the third starting point for the plague in Scania was Ystad, where on 19 June an infected soldier arrived from Swedish Pomerania. The plague remained in Scania until 1713, probably 1714
Commanding general Christopher von Stoffeln coerced army doctors to conceal the outbreak, which was not made public until Gustav Orreus, a Russian-Finnish surgeon reporting directly to Field Marshal Pyotr Rumyantsev, examined the situation, identified it as plague and enforced quarantine in the troops. Shtoffeln, however, refused to evacuate the infested towns and himself fell victim to the plague in May 1770. Of 1,500 patients recorded in his troops in May–August 1770, only 300 survived (politicking during the outbreak was followed by failure of containment.)
The disease spread by smugglers during the 1813–14 Malta plague epidemic
Cholera was endemic to the lower Ganges River. At festival times, pilgrims frequently contracted the disease there and carried it back to other parts of India on their returns, where it would spread, then subside. The first cholera pandemic started similarly, as an outbreak that was suspected to have begun in 1817 in the town of Jessore. Some epidemiologists and medical historians have suggested that it spread globally through a Hindu pilgrimage, the Kumbh Mela, on the upper Ganges River
the small-pox had never been known in the civilized world, as it had been among the poor Mandans and other Indians. Only twenty-seven Mandans were left to tell the tale
Smallpox was (may?) have been intentionally spread among the indigenous people of the Americas by colonizers.
According to the World Health Organization, the pandemic was considered active until 1960, when worldwide casualties dropped to 200 per year. A natural reservoir or nidus for plague is in western Yunnan and is still an ongoing health risk (about the bubonic plague!).
The British colonial government in India pressed medical researcher Waldemar Haffkine to develop a plague vaccine. After three months of persistent work with a limited staff, a form for human trials was ready. On January 10, 1897 Haffkine tested it on himself. After the initial test was reported to the authorities, volunteers at the Byculla jail were used in a control test, all inoculated prisoners survived the epidemics, while seven inmates of the control group died. By the turn of the century, the number of inoculees in India alone reached four million. Haffkine was appointed the Director of the Plague Laboratory (now called Haffkine Institute) in Bombay
Although many residents held the city government responsible for the virulence of the epidemic (leading to cholera riots in 1893), it continued with practices largely unchanged
American author Mark Twain, an avid traveler, visited Hamburg during the cholera outbreak, and he described his experience in a short, uncollected piece dated “1891–1892”. Therein, he notes alarmingly the lack of information in Hamburg newspapers about the cholera event, particularly death totals
The Chinese government also sought the support of foreign doctors, a number of whom died as a consequence of the disease. In Harbin, this included the Frenchman Gérald Mesny, from the Imperial Medical College in Tientsin, who disputed Wu’s recommendation of masks; a few days later, he died after catching the plague when visiting patients without wearing a mask
They would be conscious and aware – yet not fully awake; they would sit motionless and speechless all day in their chairs, totally lacking energy, impetus, initiative, motive, appetite, affect or desire; they registered what went on about them without active attention, and with profound indifference. They neither conveyed nor felt the feeling of life; they were as insubstantial as ghosts, and as passive as zombies
The pandemic disappeared in 1927 as abruptly and mysteriously as it first appeared. The great encephalitis pandemic coincided with the 1918 influenza pandemic, and it is likely that the influenza virus potentiated the effects of the encephalitis virus or lowered resistance to it in a catastrophic way
To maintain morale, World War I censors minimized early reports of illness and mortality in Germany, the United Kingdom, France, and the United States. Newspapers were free to report the epidemic’s effects in neutral Spain, such as the grave illness of King Alfonso XIII, and these stories created a false impression of Spain as especially hard hit.
A large factor in the worldwide occurrence of this flu was increased travel. Modern transportation systems made it easier for soldiers, sailors, and civilian travelers to spread the disease.[41] Another was lies and denial by governments, leaving the population ill-prepared to handle the outbreaks
In 1918, older adults may have had partial protection caused by exposure to the 1889–1890 flu pandemic, known as the “Russian flu”
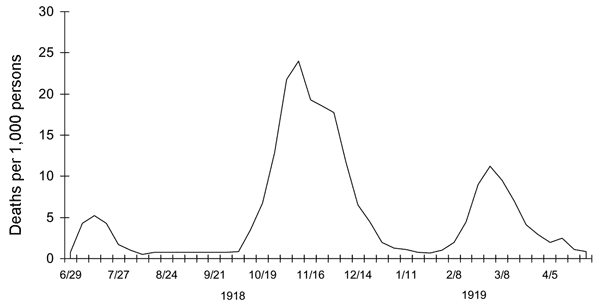
(Image for the 1918 Spanish Flu)
Another oddity was that the outbreak was widespread in the summer and autumn (in the Northern Hemisphere); influenza is usually worse in winter
In New Zealand, 8,573 deaths were attributed to the 1918 pandemic influenza, resulting in a total population fatality rate of 0.7%. Māori were 8 to 10 times as likely to die as other New Zealanders (Pakeha) because of their more crowded living conditions
Despite the high morbidity and mortality rates that resulted from the epidemic, the Spanish flu began to fade from public awareness over the decades until the arrival of news about bird flu and other pandemics in the 1990s and 2000s. This has led some historians to label the Spanish flu a “forgotten pandemic”
In 2017, Canadian scientists recreated an extinct horse pox virus to demonstrate that the smallpox virus can be recreated in a small lab at a cost of about $100,000, by a team of scientists without specialist knowledge
